Burns and Inhalational Injury
Risk flags: Assume inhalational injury
- Enclosed-space fire, explosion, prolonged smoke exposure
- Soot in mouth/nose, singed nasal hair, carbonaceous sputum
- Hoarseness, cough, wheeze/stridor, dysphagia
- Facial/neck burns, oropharyngeal edema, drooling
- Altered mental state, syncope, seizures (think Carbon Monoxide / Cyanide poisoning)
Initial actions
a. High-flow oxygen immediately (non-rebreather; do not wait for labs)
b. Remove all hot/smoldering clothing + jewelry (rings become tourniquets)
c. Warm the room, cover with warm blankets (burn patients crash fast from hypothermia)
1) Rapid Clinical Assessment & Stabilization
ABCDE approach
A - Airway:
Intubate early if any of:
- Stridor, respiratory distress, hypoxia despite O₂
- Progressive hoarseness, inability to handle secretions, significant oropharyngeal burns/edema
- Deep facial/neck burns + anticipated swelling / long transfer / limited airway backup
- Altered mental state in fire exposure (CO/CN until proven otherwise)
- Need for ongoing resuscitation/analgesia/procedures with unreliable airway
Tips
- Prefer video laryngoscopy first pass + bougie ready
- Use larger ETT if you can (adult 7.5–8.0) anticipating airway toilet/bronch
- Anticipate difficult airway; prepare surgical airway kit upfront if neck burns/edema
After intubation: secure tube well (burned face = tape failure), consider ties/ETT holder
B - Breathing:
Look for circumferential chest burns → restrictive ventilation
If ventilatory pressures rise + chest expansion limited → chest escharotomy may be life-saving
Consider early CXR and if available, bronchoscopy for diagnosis/airway toilet
C - Circulation:
Two large-bore IVs (or IO), start warmed fluids
Assess perfusion, lactate, urine output target 0.5 mL/kg/hr (adult)
D - Disability: tox until proven otherwise
Any AMS after fire: treat as CO/CN exposure while you investigate
Don’t forget to check glucose
E - Exposure + Environment
Fully expose to map burns, then re-cover quickly to prevent hypothermia
Do a full trauma sweep if blast/structural collapse
2) Assessing the Burn Severity
Depth
- Superficial: red, painful, blanches
- Partial thickness: blistering, wet/pink, very painful
- Full thickness: leathery, waxy/white/brown, insensate centrally
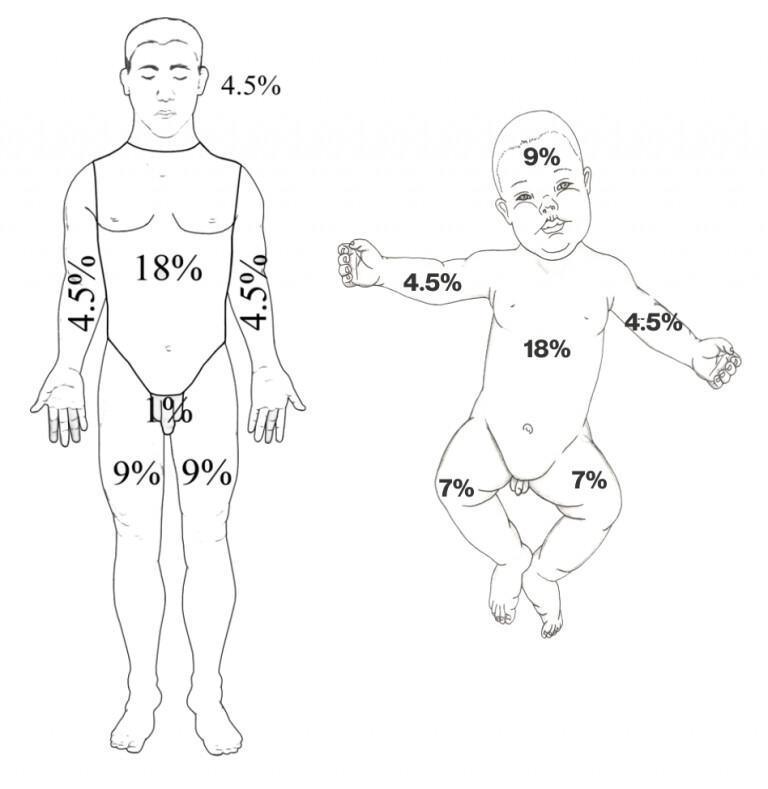
Size (TBSA)
- Use Rule of Nines (adult) or Lund-Browder (children)
- Do not count superficial erythema in TBSA for fluids
3) Inhalational Injury: treat the big two (CO + CN)
Carbon Monoxide (CO)
- Pulse oximetry can be normal.
- Send co-oximetry (carboxyhemoglobin) if available; VBG/ABG for acid-base
- Give 100% oxygen until symptoms resolve and COHb down-trending
- Consider hyperbaric oxygen discussion/transfer if any of:
- Loss of consciousness, neurologic deficits, significant cardiac ischemia/arrhythmia
- Severe metabolic acidosis, pregnancy with significant symptoms/COHb elevation
- Persistent symptoms despite high-flow O₂
Cyanide (CN)
Think CN if:
- Enclosed-space fire + severe lactic acidosis (especially very high lactate) ± AMS/collapse
- Rapid cardiovascular collapse unexplained by burn size
Treat empirically if clinical suspicion is high
Antidote commonly used: hydroxocobalamin (if available)
4) Fluid Resuscitation (for major burns)
Indication for commencing fluid resuscitation:
- Adults: ≥20% TBSA (ATLS), ≥15% TBSA (TLSM)
- Children/elderly: ≥10–15% TBSA
Fluid formula:
ATLS (modified Brooke)
2 mL × kg × %TBSA of Ringer’s lactate in first 24h
Give half in first 8h from TIME of burn
Remaining half over next 16h
TLSM (Parkland)
4 mL × kg × %TBSA of Ringer’s lactate in first 24h
Give half in first 8h from TIME of burn
Remaining half over next 16h
Titration target: urine output
Adult: 0.5 mL/kg/hr
Electrical/high-risk rhabdo: aim higher (often 1 mL/kg/hr) + monitor CK/urine
5) Escharotomy / Compartment Threat
Circumferential limb burns:
Ischemia checklist
- Pain out of proportion, paresthesia, pallor, poikilothermia
- Diminished cap refill, weak/absent Doppler signals
- Increasing tightness with swelling
Circumferential chest burns
- Rising airway pressures, hypercapnia, poor chest excursion
- Consider chest escharotomy in ventilated patient with clear restriction pattern
6) Analgesia & Sedation
Use IV opioids early (titrate to effect)
Add ketamine when pain is severe, procedures needed, or hypotension risk
7) Wound Care in ED
a. Cooling
- Cool the burn with cool running water early (best within ~3 hours), avoid ice
- Stop once pain improves; prevent hypothermia (especially kids/large TBSA)
b. Debridement & dressing
- Gently clean with saline
- Leave intact blisters if small/non-tense; de-roof if large/tense/dirty or impairing movement (local practice varies. Prioritize function + infection risk)
- Cover with clean dry dressing / cling film (non-adherent), keep warm
c. Topicals
- Avoid complicated topical regimens in the ED unless your burn service requests it
- Silver sulfadiazine is not a universal “default” (can delay healing in some partial-thickness burns and is not ideal on face)
8) Infection Prevention, Tetanus, Antibiotics
Tetanus update per wound status/immunization history
No prophylactic systemic antibiotics for uncomplicated burns
Give antibiotics only if contaminated wound, associated open injury, clear infection, inhalation pneumonia later, etc.
9) Special Burn Types
a. Electrical burns
Skin can look minor while deep tissue is destroyed
ECG + continuous monitoring; check CK, renal function, urine for myoglobin
Aggressive fluids; consider higher UO targets
b. Chemical burns
Immediate copious irrigation (minutes matter)
Remove contaminated clothing; protect staff
Identify agent
11) Burn Center / ICU Referral Triggers (transfer early)
- Inhalation injury suspected/confirmed
- Partial thickness >10% TBSA (especially children)
- Any full thickness significant area
- Face, hands, feet, genitalia, perineum, major joints
- Circumferential limb/chest burns
- Electrical/chemical burns
- Significant comorbids, extremes of age, associated trauma
- Social/functional issues preventing safe outpatient care
References
1. American Burn Association. (2022). Guidelines for burn patient referral. Journal of Burn Care & Research, 43(6), 1081–1086. https://doi.org/10.1093/jbcr/irac104
2. Atiyeh, B. S., Costagliola, M., Hayek, S. N., & Dibo, S. A. (2009). Effect of silver on burn wound infection control and healing: Review of the literature. Burns, 35(2), 139–148. https://doi.org/10.1016/j.burns.2008.06.010
3. Sartorelli, K. H., & Shapiro, M. B. (2023). Initial management of moderate and severe thermal burns in adults. In UpToDate. Wolters Kluwer.
4. National Comittee on Resuscitation Training (NCORT). (2025). Trauma Life Support Malaysia (TLSM) student provider manual. TLSM Malaysia.
5. Weaver, L. K. (2014). Clinical practice. Carbon monoxide poisoning. The New England Journal of Medicine, 360(12), 1217–1225. https://doi.org/10.1056/NEJMcp0808891